Key Takeaways
- The global generative AI market is projected to reach $39.70 billion by 2034, showing a CAGR of 35.17%. This is capital following demonstrated results, not speculation.
- Ambient scribing, prior authorization automation, and administrative intelligence deliver measurable, near-term returns with relatively low regulatory complexity.
- Real-world deployments are already producing results. Companies like Insilico Medicine, Nuance, and Aidoc are not running pilots — they are operating at scale.
- Data fragmentation, regulatory complexity, the talent gap, and clinician adoption are the four most common points of failure.
- The next 24 months will see multimodal diagnostics, point-of-care ambient intelligence, and clinical-specific foundation models move from early adoption to standard infrastructure.
Healthcare operations are moving at a fast pace. With patients demanding user-friendly, accessible medical care services now more than ever, businesses are expected to adapt to this change quickly.
What required years of clinical iteration now compresses into months of model training. And generative AI in healthcare is rewriting the code of medicine itself. For years, healthcare has been data-rich but insight-poor. Electronic health records, imaging systems, genomics platforms, claims databases — all generating signals. Yet the system struggled to synthesize them in real time. Generative AI is beginning to close that gap.
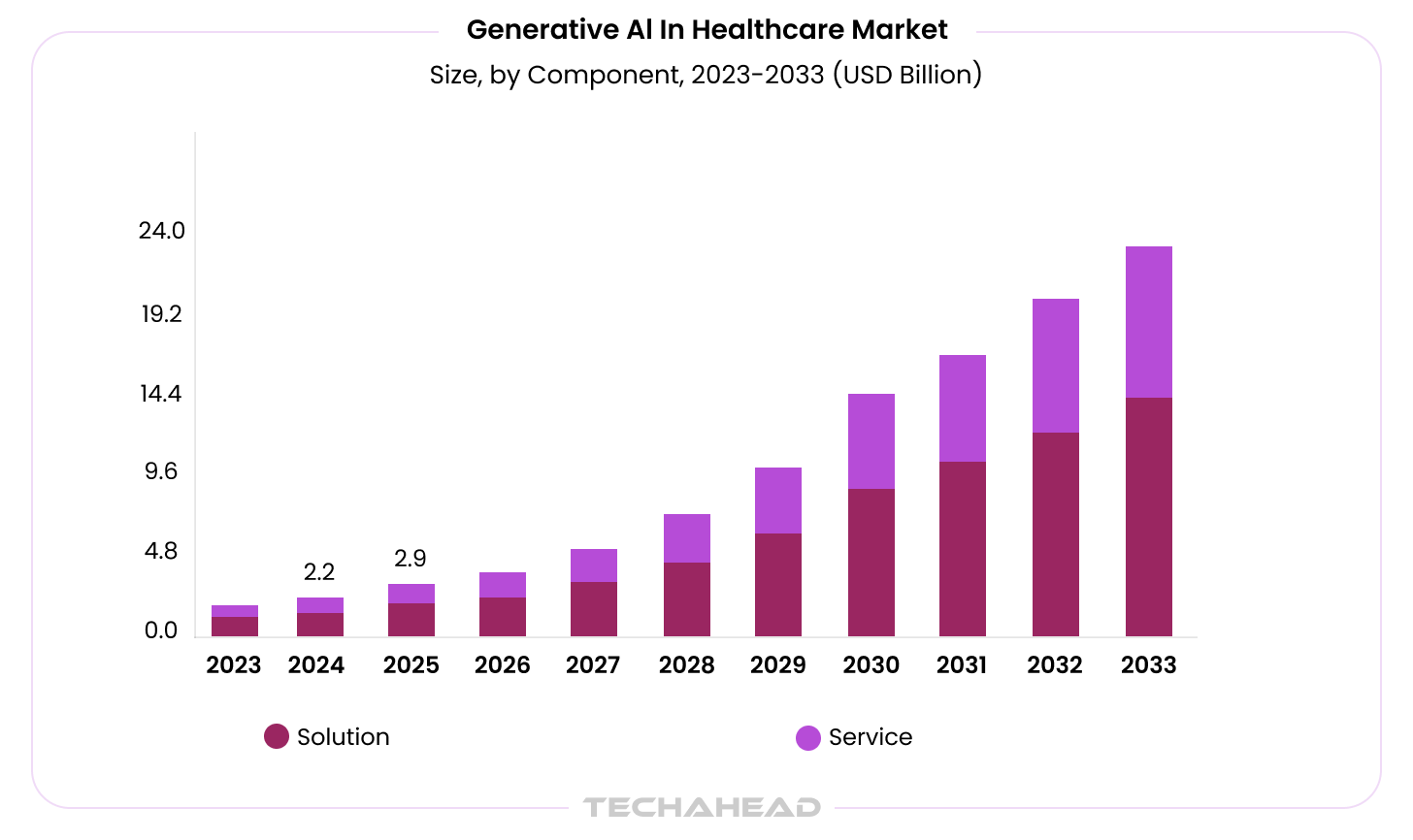
The global generative AI in healthcare market is valued at USD 2.64 billion in 2025 and projected to reach approximately USD 39.70 billion by 2034, expanding at a CAGR of 35.17%. That growth is not driven by experimentation. It is driven by operational adoption.
Hence, Gen AI in healthcare is no longer a future bet. It is a present competitive advantage for organizations that move decisively.
Why Generative AI in Healthcare: The Shift That’s Already Happening
Traditional AI—think rule-based systems or predictive models like random forests—excelled at pattern-matching but choked on nuance, context, or unstructured data. They predicted heart failure risk from clean vitals but could not weave in a patient’s social history or generate a hypothesis from blurry scans.
Implementing generative AI in healthcare changes that equation.
Where predictive systems flag risk, generative systems synthesize fragmented data, generate insights, and support reasoning across modalities. Language models interpret clinical notes. Multimodal systems process imaging, labs, and genomics together. Diffusion and transformer architectures generate molecules, documentation, and treatment hypotheses.
The momentum is measurable. In a late-2024 industry survey of healthcare leaders across payers, health systems, and healthcare services and technology organizations, 85% reported that they were either actively exploring or had already implemented gen AI capabilities. Adoption is no longer experimental. It is strategic.
This is not a research lab conversation anymore. It is an enterprise operations conversation.
Healthcare organizations are embedding generative AI in clinical documentation, diagnostics, drug discovery, and patient engagement workflows. The shift is underway — not as a pilot trend, but as a foundational technology transition.

What Generative AI Actually Does in a Clinical Environment
Stripped of hype, gen AI applications in healthcare revolve around three enterprise-relevant capabilities:
- Synthesis
Healthcare data is fragmented across systems. Generative AI synthesizes EHR records, imaging, genomics, and structured data into coherent summaries and actionable insights.
- Generation
From clinical documentation to discharge summaries to drug candidates, generative systems create structured outputs from unstructured input.
- Prediction with Context
Not just flagging risk, but anticipating patient trajectories using longitudinal reasoning across multimodal data.
What this is not: a replacement for clinicians.
What it is: a compression layer between data and decision.
Generative AI Use Cases in Healthcare That Are Delivering Results Now
From the moment a patient enters the system to how organizations operate behind the scenes, you can find generative AI use cases in healthcare operations. These are no longer pilot programs or POC deployments. They are live, scaling implementations producing measurable outcomes.
Predictive Diagnostics
Earlier computer vision systems flagged anomalies. Generative systems reason across incomplete data and generate differential diagnoses — synthesizing context, not just detecting patterns. This is not automation. It is augmented clinical reasoning at scale. Predictive diagnostics is among the most mature gen AI in healthcare use cases today.
What’s happening:
- AI-assisted radiology and pathology systems trained on millions of scans
- Automatic abnormality detection and urgent case prioritization
- Preliminary interpretation drafting
- Risk stratification models across oncology, cardiovascular, and neurological domains
Enterprise impact:
- Shorter scan-to-decision windows
- Improved triage accuracy
- Intervention at the earliest clinically meaningful moment
Personalized Treatment Planning
Decision-making moves from manual synthesis to AI-assisted structuring. Cognitive load decreases. Speed increases. Consistency improves. Hence, personalized medicine has long been aspirational. Generative AI makes it operational.
These gen AI applications in healthcare are redefining what “personalized” means in practice.
What’s happening:
- LLMs synthesizing clinical history, genomics, medication profiles, and guidelines
- Structured treatment recommendations surfaced in real time
- Automated drug interaction analysis
- Dosage personalization based on patient-specific variables
Enterprise impact:
- Scalable precision medicine
- Improved patient stratification in trials
- Data assets that compound in value over time
Clinical Documentation and Administrative Intelligence
Documentation is one of healthcare’s largest hidden cost centers. Generative AI in healthcare reduces administrative drag while improving data completeness.
What’s happening:
- Ambient AI scribing during patient visits
- Automated coding and billing support
- Prior authorization drafting
- Discharge summary generation
Enterprise impact:
- Reduced clinician burnout
- Faster reimbursement cycles
- Higher data quality across EHR systems
Drug Discovery and Development
Generative AI is revolutionizing drug discovery and development by shifting from compressing early discovery phases that have consumed years. Gen AI makes research pipelines computationally iterative rather than purely experimental.
What’s happening:
- Novel molecule generation
- Protein interaction prediction
- Synthetic research data generation
- Trial design optimization
Enterprise impact:
- Shorter discovery cycles
- Reduced attrition in early candidates
- Higher scientific throughput
Patient Engagement and Virtual Care
Not every patient in interaction requires a clinician, but every interaction requires context-aware intelligence. These applications of generative AI in healthcare extend clinical intelligence beyond hospital walls.
What’s happening:
- Conversational symptom assessment
- Chronic disease management support
- Medication adherence coaching
- Proactive outreach based on risk signals
Enterprise impact:
- Expanded care capacity without proportional workforce expansion
- Continuous engagement between visits
- Improved outcomes in chronic populations
Operational and Supply Chain Intelligence
These gen AI use cases in healthcare may not headline conferences, but they deliver measurable financial leverage.
What’s happening:
- Predictive staffing models based on patient volume forecasts
- Claims anomaly detection at scale
- Resource allocation optimization
- Supply chain demand forecasting
Enterprise impact:
- Cost containment
- Fraud reduction
- Crisis prevention before shortages materialize
Real-world Examples of Generative AI in Healthcare
The generative artificial intelligence in healthcare examples that matter most to enterprise decision-makers are not the ones being theorized — they are the ones already in deployment. Here are seven organizations whose work defines what is actually possible right now.
Insilico Medicine
- Uses generative AI to design novel drug candidates from scratch.
- Generated INS018_055, a fibrosis treatment, which reached Phase II clinical trials.
- The molecule was identified and optimized using generative AI before laboratory synthesis and validation.
Nuance Communications — Dragon Medical One
- Generates structured clinical notes directly from physician-patient conversations using ambient AI scribing.
- Significantly reduces documentation burden, returning meaningful time to clinicians.
- One of the most widely deployed examples of generative AI in healthcare administrative settings globally.
Aidoc
- Flags urgent radiology cases in real time and identifies critical imaging findings.
- Enables radiologists to prioritize time-sensitive cases without manual case sorting.
- Supports faster clinical response in conditions where time to treatment directly impacts outcomes.
Syntegra
- Generates synthetic patient datasets that are statistically representative of real populations.
- Enables clinical research, model training, and analytics while reducing reliance on identifiable patient data.
- Addresses one of the most persistent barriers to AI development in healthcare: the tension between data access and privacy.
What a Responsible Gen AI Deployment in Healthcare Systems Actually Looks Like
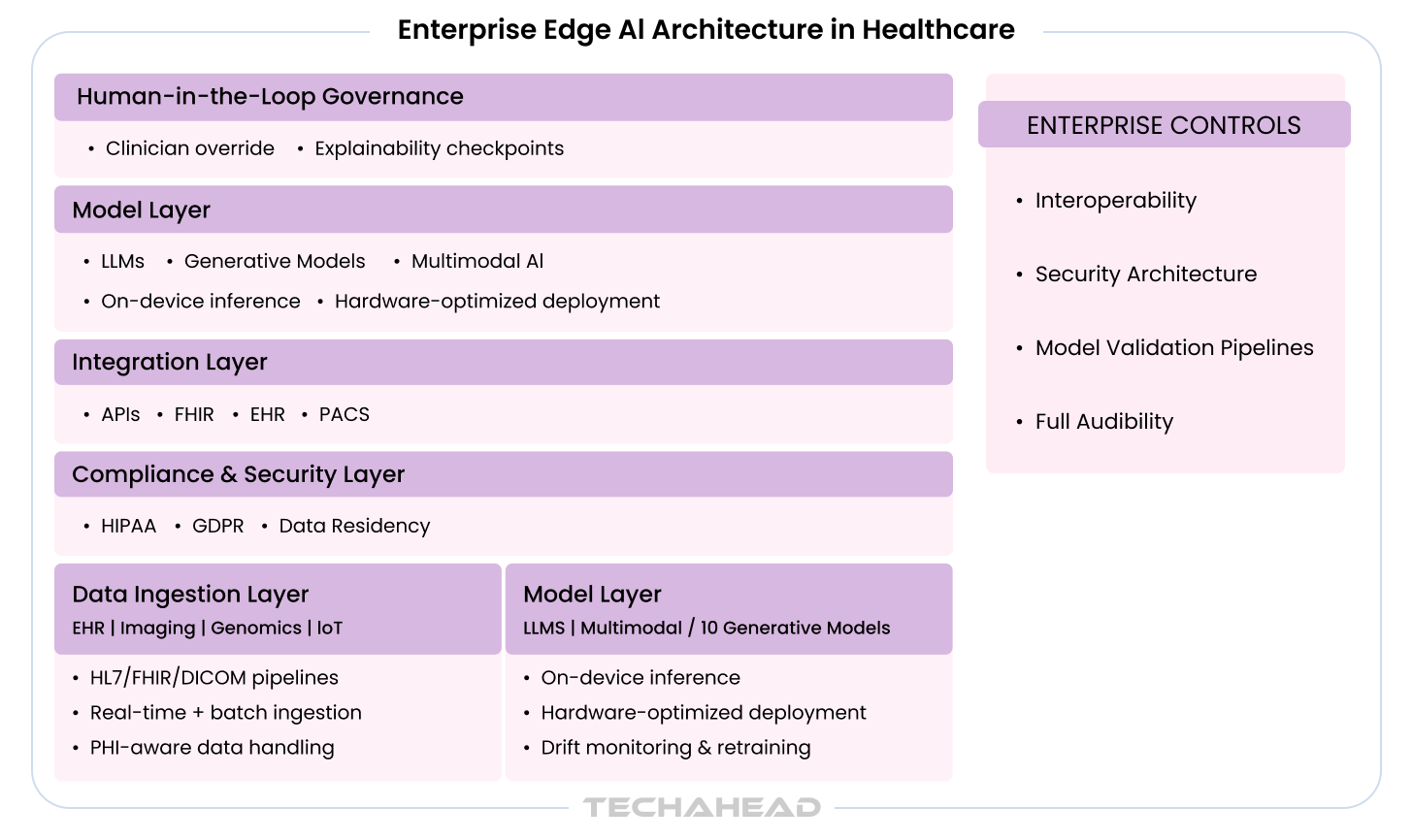
The organizations that extract durable value from Generative AI investments share a common discipline: they treat deployment as a structured process, not an accelerated experiment.
Discovery and Use Case Prioritization
The right starting point of generative AI in healthcare deployment is a rigorous assessment of where the combination of data availability, clinical impact, and implementation complexity creates the best risk-adjusted return. Clinical documentation is frequently the right first move — high impact, relatively low regulatory complexity, and fast feedback loops.
Data Readiness Assessment
Generative AI models perform according to the quality of the data they work with. EHR data is often fragmented, inconsistently structured, and siloed across systems that were never designed to speak to each other. An assessment of data infrastructure determines what is buildable on what timeline. Organizations that skip this step tend to discover the gap at the worst possible moment.
Model Selection and Customization
The build-versus-buy-versus-fine-tune decision is consequential. Foundation models from major providers offer significant capability out of the box, but clinical applications frequently require fine-tuning on domain-specific data to reach the accuracy and safety thresholds that healthcare demands. Most enterprise deployments end up with a hybrid approach, using third-party foundation models for speed while customizing clinical specificity.
Validation and Clinical Testing
Pilots need to generate real evidence measured against clinical outcomes, workflow efficiency, and user adoption. This phase is where many organizations stall, because they launch pilots without clear success criteria. Define what good looks like before the pilot starts, not after it ends.
Regulatory and Compliance Integration
HIPAA data use requirements, FDA guidance on AI-assisted clinical decision support, and emerging frameworks like the EU AI Act all have implications for how models are trained, validated, and monitored.
Governance cannot be a final checkpoint. It needs to be embedded from the beginning. Organizations that treat it as an afterthought create expensive rework cycles that delay deployment and erode stakeholder confidence.
Deployment and Monitoring
Go-live is not a finish line. Model drift, where performance degrades as real-world data patterns shift from training conditions, is a genuine operational risk. Continuous monitoring, explainability mechanisms, and structured feedback loops with clinical users are not optional. They are part of the operational model.

Challenges Associated with Implementing Generative AI in Healthcare
The barriers to generative AI adoption in healthcare are real, and leaders who understand them clearly are better positioned to navigate them than those who discover them mid-deployment. Here is an honest accounting of what the implementation landscape actually looks like.
Data Fragmentation
EHR interoperability remains the single most common structural blocker for gen AI in healthcare implementations. Most health systems operate with patient data distributed across multiple platforms, in inconsistent formats. This limits the capability of generative AI to perform at its potential.
Solution: Requires infrastructure investment that needs to precede or run in parallel to AI deployment, not follow it.
Regulatory Complexity
The FDA’s evolving framework for AI and machine learning-based software, HIPAA’s data use and privacy requirements, and the EU AI Act’s risk classification system for healthcare AI all create genuine complexity for enterprise deployments.
Solution: Build compliance capacity as a core component of the deployment team and engage with regulatory guidance proactively rather than reactively.
The Talent Gap
The actual capability gap sits at the intersection of clinical knowledge, data science, and enterprise implementation experience.
Solution: Hire a strategic healthcare application development company with specialized vendors or technology consultancies, particularly for organizations earlier in their AI maturity curve.
Clinician Adoption
A healthcare generative AI tool that clinicians do not trust or do not use delivers no value, regardless of its technical sophistication, and is a significant challenge.
Solution: Change management and transparent communication about how models were validated are primary determinants of whether a deployment succeeds or stalls.
Future Trends for Generative AI in Healthcare — What the Next 24 Months Look Like
The trajectory of gen AI in healthcare over the next two years is becoming clear. The organizations that are positioning it now will have a meaningful advantage over those that wait for trends to fully materialize before responding.
- Multimodal AI integrating text, imaging, genomics, and wearable data.
- Ambient intelligence embedded at the point of care.
- Healthcare-specific foundation models are gaining traction.
- Regulatory clarity is accelerating enterprise deployment.
- Convergence of generative AI with edge computing in remote and rural settings.
- Personalized medicine is becoming operational at scale.
Gen AI in healthcare is moving from the application layer to the infrastructure layer.
The Real Question Is Not “Should We?” — It’s “How Fast?”
Generative AI in healthcare is not an experimental horizon. It is already reshaping diagnostics, documentation, drug discovery, and patient engagement. Therefore, the time for collaborating with a company that offers generative AI development services is now.
The organizations that define care delivery over the next decade should be asking these three questions:
- Where in our current workflows is the distance between data and decision costing us the most?
- What does our data infrastructure’s honest readiness for gen AI deployment actually look like?
- Who owns this initiative strategically?
The window for cautious observation is narrowing. It requires executive ownership, cross-functional alignment, and a time horizon long enough to see the compounding returns materialize. The organizations building that capability now are not just staying competitive with the field — they are defining what the next standard of care looks like.

The highest-value, fastest-return gen AI use cases in healthcare for enterprise health systems today are clinical documentation automation, predictive diagnostics in radiology and pathology, and operational intelligence, including predictive staffing and claims fraud detection. Drug discovery and personalized treatment planning carry larger long-term value but require deeper data infrastructure and longer deployment timelines.
The cost structure spans four areas: infrastructure, model development or licensing, clinical validation and compliance, and ongoing monitoring and operations. Early-stage implementations are significantly less capital-intensive than full clinical AI platforms. The more useful framing is not upfront cost but value against reduced administrative burden, faster diagnosis, shortened R&D cycles, and improved patient throughput.
A focused, well-scoped deployment can reach production within three to six months with the right partner and data readiness. More complex clinical applications involving diagnostic support or drug discovery integration operate on 12 to 24-month timelines. Timeline is largely determined by data readiness and organizational change management, not just the technology build itself.
HIPAA-compliant generative AI deployments require data de-identification or appropriate user agreements, secure infrastructure with access controls, and audit logging. Additionally, it needs business associate agreements with any third-party model providers and model training practices that prevent patient data from leaking into general-purpose models. Any healthcare AI development company worth engaging should be able to walk you through their compliance framework in detail before a contract is signed.
Most enterprise deployments end up with hybrids. Off-the-shelf platforms offer faster time to value for well-defined use cases like documentation or basic patient engagement. Custom builds offer control, differentiation, and the ability to train on your proprietary clinical data. The decision framework should be based on how strategically differentiated the capability needs to be, how unique your data assets are, and how much ongoing customization the use case requires.
Five risks that enterprise leaders need to own explicitly: model hallucination in clinical contexts, data bias, regulatory non-compliance, clinician distrust, and model drift. Hence, you should deploy generative AI healthcare solutions with rigor.



